Definition
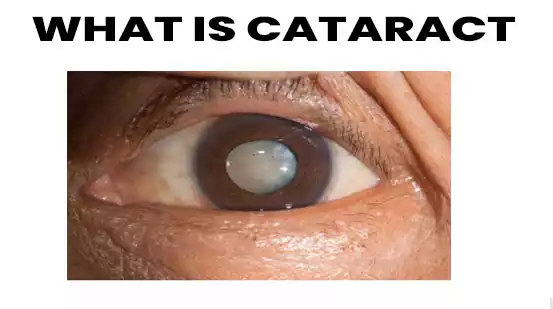
- A cataract is a disorder in which opacity (cloudiness) in the lens of the eye and degeneration of lens fibers, lead to blurred vision.
- A cataract occurs due to hydration, denaturation of lens protein, and sclerosis.
-
A cataract is the most common cause of blindness.
Cataract classification
-
According to etiology
-
Acquired cataract
- Acquired cataracts commonly occur.
- Acquired cataract are
- Senile cataract
- Metabolic cataract
- Complicated cataract
- Traumatic cataract
-
Cataracts
associated with skin disease
- Drug Induced cataract
- Cataract with miscellaneous syndrome
- Electric cataract.
-
Developmental cataract
- Also known as the congenital cataract occurs due to disturbance in normal development of the lens.
- Generally development cataracts occur in the infancy to adolescence, due to genetic disorders.
2. According to morphology
- Subcapsular cataract – anterior subcapsular cataract.
- Posterior subcapsular cataract.
-
Cortical cataract –
a cataract occurs due to wedge shape or radial spoke like opacities of lens.
- Occur outer edge of the lenses.
-
Nuclear cataract –
a cataract occurs in the center of the lens.
- Yellow to Brown coloration.
Causes of Cataract

- Hereditary
- Family history
- Age factors
- Malnutrition during pregnancy
- Radiation exposure
- Excessive use of corticosteroids
- Down syndrome
- Skeletal syndrome
- Chromosome abnormality
- Birth trauma
- Infection
- Diabetes mellitus
- Trauma
- Marfan syndrome
- Previous ocular surgery
- Wilson disease.
Pathophysiology of Cataract
Cause / Etiology
↓
Traumatic damage the lens fibres
↓
Rupture lens capsule
↓
Hydration of lens fibers
↓
Opacity of lens.
Signs/Symptoms of Cataract
Clinical manifestation of
Cataract Clinical manifestation
- Cloudy vision
- Blurred vision
- Photophobia ( sensitive to light )
- Double vision
- Monocular diplopia
- Glare
- Distortion of lines
- Reduce visual acuity
- Dim red reflex
- Poor vision at night
- Decrease colour perception
- White pupil.
Diagnostic examination of Cataract
- History collection and physical examination.
- Direct ophthalmoscope examination.
- Snailing visual acuity test.
- Slit lamp examination.
- Tonometry.
- Retinal examination.
Medical management of Cataract
- Use glasses
- Optical aids
- Pupillary dilation
- Topical steroids
- Antibiotics drops
- Steroid drops.
Surgical management of Cataract
- Intracapsular extraction – remove the whole lens and surround it.
- Extracapsular extraction – only cataract removal.
- Cryosurgery
- Phacoemulsification – emulsifying of the lens by a hollow needle vibrating and ultrasonic speed.
Complication – Blindness.
Nursing management
- Nurses monitor patients’ visual acuity and vital signs.
- Examine the complete morphology of lens opacity under slit lamp examination.
- Examine the cornea to find out any opacity of the lens.
- Monitor intraocular pressure (IOP).
- Nurses also assess pupillary response.
- The nurse performed the cover test.
- Use a nursing barrier to prevent infection.
- Nurses assist the client during any activity.
- Provide instruction about cataract patient care and Management.
- Nurses help to conduct diagnostic examinations.
- Provide adequate medications and other required treatment.
- Provide emotional and physiological support and reduce anxiety.
- Prepare the client for surgical intervention.
- Administer local anesthesia with sedation before surgery.
- Nurse counseling to relieve patient anxiety.
What is the main cause of cataracts?
Hereditary
Family history
Age factors
Malnutrition during pregnancy
Radiation exposure
Excessive use of corticosteroids
Down syndrome
Skeletal syndrome
Chromosome abnormality
Birth trauma
Infection
Diabetes mellitus
Trauma
- a16z generative aiHippocratic AI raises $141M to staff hospitals with clinical AI agents Story Partners with Stability AI to Empower Open-Source Innovation for Creators and Developers Meanwhile, Kristina Dulaney, RN, PMH-C, the founder of Cherished Mom, an organization dedicated to solving maternal mental health challenges, helped to create an AI agent that’s focused on helping new mothers … Read more
- a16z generative aiHippocratic AI raises $141M to staff hospitals with clinical AI agents Story Partners with Stability AI to Empower Open-Source Innovation for Creators and Developers Meanwhile, Kristina Dulaney, RN, PMH-C, the founder of Cherished Mom, an organization dedicated to solving maternal mental health challenges, helped to create an AI agent that’s focused on helping new mothers … Read more
- TestTest link
- ai in finance examples 1Top AI Tools for a Finance Professional Top Artificial Intelligence Applications AI Applications 2025 Banks must also evaluate the extent to which they need to implement AI banking solutions within their current or modified operational processes. It’s crucial to conduct internal market research to find gaps among the people and processes that AI technology can … Read more
- ai in finance examples 1Top AI Tools for a Finance Professional Top Artificial Intelligence Applications AI Applications 2025 Banks must also evaluate the extent to which they need to implement AI banking solutions within their current or modified operational processes. It’s crucial to conduct internal market research to find gaps among the people and processes that AI technology can … Read more
- ai in finance examples 1Top AI Tools for a Finance Professional Top Artificial Intelligence Applications AI Applications 2025 Banks must also evaluate the extent to which they need to implement AI banking solutions within their current or modified operational processes. It’s crucial to conduct internal market research to find gaps among the people and processes that AI technology can … Read more
- best name for dog 74The Best Unique Boy Dog Names Perfect For Your New Pup 100 Most Popular Dog Names in 2024 2025: By Breed, State, and More P You’ve stocked up on dog food, picked the perfect leash and collar, and dog-proofed your home. About My Dog’s NameFounded in October 2013, My Dog’s Name provides a fun, interactive … Read more
Test Post for WordPress
This is a sample post created to test the basic formatting features of the WordPress CMS. Subheading Level 2 You can use bold text, italic text, and combine both styles. Bullet list item #1 Item with bold emphasis And a link: official WordPress site Step one Step two Step three This content is only for … Read moreTest Post for WordPress
This is a sample post created to test the basic formatting features of the WordPress CMS. Subheading Level 2 You can use bold text, italic text, and combine both styles. Bullet list item #1 Item with bold emphasis And a link: official WordPress site Step one Step two Step three This content is only for … Read moreTest Post for WordPress
This is a sample post created to test the basic formatting features of the WordPress CMS. Subheading Level 2 You can use bold text, italic text, and combine both styles. Bullet list item #1 Item with bold emphasis And a link: official WordPress site Step one Step two Step three This content is only for … Read more- Importance of Communication in NursingWhat is Communication Communication is derived from the Latin word “Communicare” or “communico” both. Communication is a simple form that transfers ideas, thoughts, and information from one person to another person. Communication is a process in which a message is transmitted from the sender to the receiver. Communication helps in the mutual interchange of ideas, … Read more
- 5000+ RRB Staff Nurse Previous Year Question Paper pdf downloadThe Railway Recruitment Board (RRB) 5000+ RRB Staff Nurse Previous Year Question Paper pdf download. The Railway Recruitment Board (RRB) is expected to release recruitment notifications for the Staff Nurse position soon. Candidates interested in applying for the RRB Staff Nurse Recruitment can do so on the official RRB website. Additionally, candidates are advised to … Read more
- Easy & Simple ways to improve the digestive system in 5 DaysEasy & Simple ways to improve the digestive system in 5 Days. these steps help in improving your digestive health so please note these tips in your not book and follow these steps for at least 5 days for better results. Hi Friends My Name is Pradeep Kumar I am a medical and health freak … Read more
- How to use PPE kit | PPE Kit का उपयोग कैसे करें HindiCOVID-19 देखभाल के लिए व्यक्तिगत सुरक्षा उपकरण [PPE] का उपयोग कैसे करें What is Personal Protective Equipment (PPE) पर्सनल प्रोटेक्टिव इक्विप्मेंट्स (पीपीई) सुरक्षात्मक गियर हैं जिन्हें स्वास्थ्य की सुरक्षा के लिए बनाया गया है एक जैविक एजेंट के संपर्क को कम करके श्रमिक। [Components of PPE ] पीपीई के घटक पीपीई के घटक गॉगल्स, फेस-शील्ड, … Read more
- Most Common Nursing Diagnosis List PDFActivity Intolerance:- Insufficient physical or psychological energy to endure or complete needed or desired daily activities. Acute Confusion:- Abrupt onset of a cluster of worldwide, transient changes and disturbances in attention, cognition, bodily process activity, level of consciousness, or the sleep/wake cycle. Acute Pain:- Unpleasant sensory associate degreed emotional expertise arising from actual or potential … Read more